Colic can affect any horse at any time and it can be life-threatening. Vet Imogen Burrows, from Cliffe Equine Clinic, explains what signs to look for and what to do when it strikes

Colic is one of those things all horse owners dread and most horses will suffer from at some point in their lives. It’s certainly common for vets to be called out for this problem, with around 7% of horses coming down with it each year.
Many people think of colic as a condition in itself, but it’s actually just a term that describes abdominal pain or tummy ache and can have several causes. Horses have a limited number of ways they can express pain or discomfort and colic is a catch-all term for the behaviours generally associated with this type of pain.
Signs of colic in horses
Common signs associated with colic include…
- pawing the ground
- curling or lifting the upper lip (Flehmen response)
- trying to lie down
- rolling
- sweating
- flank watching
- loss of appetite
- standing as if to urinate (lordosis)
- unsettled behaviour such as constantly switching from resting one hindleg to the other
- kicking at abdomen with hindlegs
- absence of droppings
The signs vary between individuals, depending on how stoic they are and the degree of bowel distention, inflammation of the intestinal wall and compromise to the intestinal blood supply.
Horses with an impaction usually appear dull, lose their appetite and won’t have passed droppings for several hours. Cases with a twisted bowel and an inflamed, bloated section of intestine that has a restricted blood supply are often in a huge amount of pain, responding very poorly to pain relief.
Did you know?
Fortunately, the vast majority of colics are simple cases, resolving either without veterinary attention roughly 30% of the time or after one veterinary treatment. Around 10–15% of colics are repeat cases, with some horses having multiple episodes each year.
Different types of colic
Very broadly, colic can be separated into two categories – medical and surgical.
Medical colic is defined as cases that don’t require surgical intervention as a part of treatment and includes…
- spasmodic colic, when the bowels contract abnormally causing intense, painful contractions
- ileus is where the gut movement slows significantly so food doesn’t move along it properly
- impaction is a blockage in the bowel, usually caused by a build-up of food
- false colics are cases of abdominal pain not caused by a problem in the gastrointestinal tract, such as equine exertional rhabdomyolysis (azoturia) or abortion
Medical cases are by far the most common, accounting for 90–95% of all colics. Spasmodic and simple ileus cases with no specific diagnosis account for 80–85% of all colics, and impactions occur around 10% of the time.
Surgical colic occurs when medical treatment fails and surgery is needed to resolve the problem. Non-strangulating obstructions or strangulating diseases requiring surgery account for the approximately 5% of cases remaining…
- non-strangulating obstructions that require surgery include masses within the abdomen that compress the gut externally, preventing the passage of food, and masses within the bowel that can’t be cleared medically, such as a foreign body.
- strangulating disease occurs when the blood supply is cut off to a section of bowel and, if not treated, can rapidly progress to bowel death. Severe displacement of the bowel, or twisting of the gut around itself or another object, can lead to the bowel becoming strangulated. The intestine is supported in the abdomen by a thin, mesh-like structure known as the mesentery. Occasionally, tears can occur in this structure and the bowel may pass through these holes and become strangulated.
Strangulating obstructions carry the highest fatality rate of all types of colic. Large colon torsions (twists) are the most common type of strangulating obstruction, with small intestinal strangulations the next most frequent.
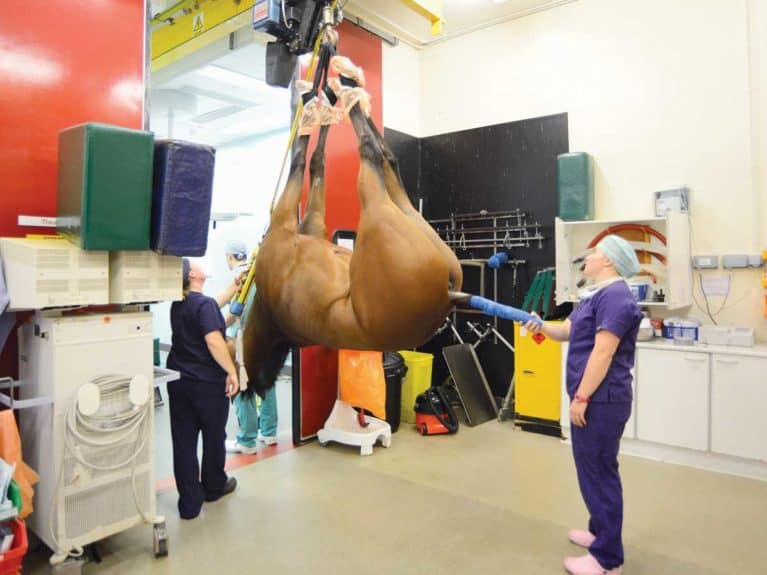
Is my horse at risk from colic?
Several factors can play a role in the likelihood of a specific type of colic occurring…
Horse factors
- Older horses are at risk of pedunculated lipomas. These are fatty masses that hang from a stalk, which can become wrapped around the intestine, causing strangulation
- Crib-biters and windsuckers are prone to large colon displacement, impaction and epiploic foramen entrapment, which is where part of the small intestine becomes trapped in a small opening in the abdomen
- Donkeys can get pelvic flexure impaction, which is a type of impaction that occurs in an area of the large colon that’s narrow and has a hairpin bend
- Warmblood types can be prone to nephrosplenic entrapment, which is where the large colon migrates between the spleen and abdominal wall, and becomes trapped
- Stallions and colts are at risk of inguinal hernia, which is where the small intestine moves into the inguinal canal (which holds the spermatic cord) and becomes strangulated
- Pregnant mares can suffer with uterine torsion, which is where the uterus becomes twisted
- Recently foaled mares are prone to large colon displacement or torsion, rupture of the uterine artery, bruised or ruptured internal organs and impaction
Management factors
- Poor dental care can lead to pelvic flexure impaction and stomach impaction if food isn’t chewed properly
- Recent box rest puts horses at risk of pelvic flexure impaction and large colon displacement or torsion because of diet change and lack of exercise
Seasonal factors
- Spring and autumn are key times for large colon displacement because of management and diet changes
- Winter is often a time for large colon impactions because of more time spent in the stable, with a sudden decrease in exercise and turnout
Geographical factors
- Sandy soils, because sand can accumulate in the gut and cause impaction
- Specific grazing that has a high risk of horses contracting certain diseases that cause colic signs, such as grass sickness
If your horse has colic
It’s always sensible to take feed or hay away from your horse, although you can offer him water. Your vet will offer some advice on the phone while they’re travelling to you. Depending on the signs your horse is showing, they may advise you to take him into a paddock or arena and walk him steadily or, for safety’s sake, to put him in a stable and leave him until they arrive.
When your vet arrives, it’s very useful for them to know…
- when your horse was last seen behaving normally
- what his appetite was like until this episode
- whether he’s passed droppings in normal quantity and form, and when
- if there have been any changes in the colic signs
- whether he has any vices such as crib-biting or windsucking
- if there have been any recent changes to his management, such as box rest, new feed or increased exercise
- if your horse has a history of colic
- if he’s travelled in the last 24 hours
- his worming history
- when his last dental examination was
- any recent or current medication
Top tip
Owners often worry about when to call their vet for colic, but vets never mind receiving a call about a colicking patient and would much rather you rang to discuss the problem sooner rather than later, so get in touch as soon as you suspect colic.
Veterinary attention
Investigation into colic starts with a thorough clinical examination by your vet. Once they’ve assessed your horse’s level of pain, they’ll…
- check his head and gums for signs of trauma, hydration and septic shock
- examine his chest and abdomen with a stethoscope to take heart and respiratory rates, rule out other diseases and assess intestinal movement
- take his temperature
- check his digital pulse in each leg
- perform a rectal examination to identify any displacement or impaction

Did you know?
Sometimes colicking horses who are in a lot of pain need to be sedated so they can be examined and treated safely.
This appraisal will give your vet an idea of how severe the colic is and act as a guide to assess your horse’s response to treatment. Depending on the findings of the initial examination and how much pain your horse is in, your vet may also perform…
- nasogastric intubation, which involves passing a tube into the stomach via the nostril to check for excess fluid accumulation in the stomach
- a blood sample to check organ function and for inflammation, infection or dehydration
- abdominocentesis, which involves drawing off abdominal fluid by inserting a needle into the underside of the abdomen so it can be checked for inflammation, infection or contamination
- rectal and transabdominal ultrasonography to examine the intestines and organs in the abdomen
- exploratory laparotomy, which involves opening up your horse’s abdomen surgically so your vet can assess all his organs
Treatment depends greatly on the type of colic diagnosed or suspected and, even then, every case is different so a treatment plan is created on a case by case basis. However, as a general rule…
- he’ll need some form of pain relief
- for cases of spasmodic colic, smooth muscle relaxants can be given to ease intestinal cramps
- ileus cases can be given medication that increases contractions in the small intestine to stimulate the gut to move again
- intravenous fluid therapy (drip) is often given when the horse is in shock or dehydrated
- cases of impaction colic are often given fluids via nasogastric intubation to wet down the food blockage and allow it to pass
Life after colic
The vast majority of colic cases are mild and respond to treatment very quickly and successfully. However, sometimes surgical intervention is necessary. Surgery is often successful, although the risk of colic occurring in the future is higher due to adhesions forming within the abdomen as a result of the operation.
Many horses have one bout of colic and never suffer again, however some are more prone to it. If your horse has three or more episodes of colic in a matter of months, it definitely warrants further investigation to find the cause.













