Mud fever is the bane of many horse owners’ lives during the winter months. Vet Kate Maxwell from Severn Edge Equine Vets explains what to look for, how to treat it and, most importantly, how to prevent it setting in

Mud fever is a complicated skin reaction that affects horses’ lower legs and has many different causes. It is more correctly termed equine pastern dermatitis, but is also called greasy heel or cracked heel, and is most commonly the result of a bacterial infection by Dermatophilus congolensis, although there are a number of other organisms that contribute to the disease.
As the name suggests, mud fever is most frequently seen in horses during wet, muddy conditions, but this is not always the case. The condition is more common on the hindlegs and tends to affect the back of the pastern, causing an inflamed, scabby area that may be itchy and painful. It is more common in the feathered breeds, but can affect any horse, pony or donkey.
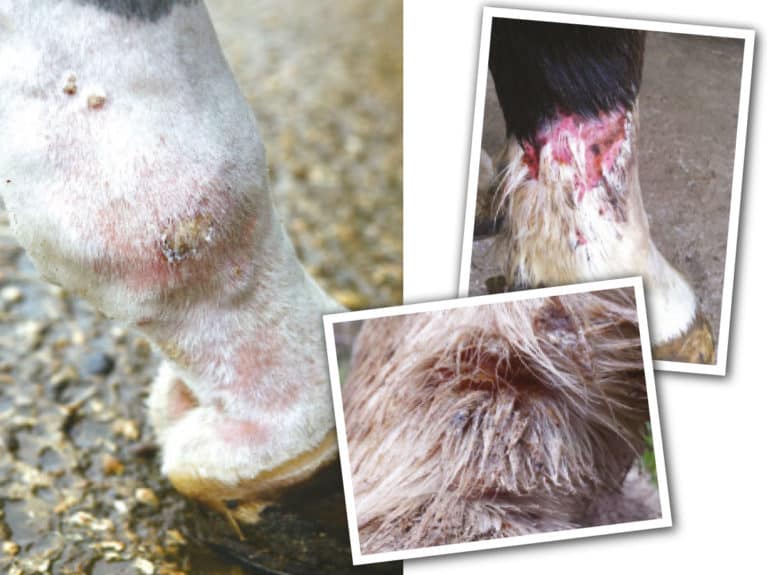
Know the signs of mud fever
The first signs of mud fever are inflammation and thickening of the skin at the back of the horse’s pastern or heel. This can then progress around and up the leg. The lesions usually only go as far as the fetlock, but in extreme cases the whole lower leg can be affected.
To begin with, there may be some hair loss and crusting, but as the infection progresses, this becomes more pronounced within the horizontal skin folds. There may be a wet, greasy look to the leg where serum oozes from the affected skin and this may progress to a white, pus-like discharge. These discharges dry and harden into thick crusts that harbour the bacteria. More severe cases will become very painful, the whole lower limb will become swollen and hot, and the horse may become lame.
Occasionally, the bacteria may also infect skin over the quarters and along the back of a horse, causing scabs that look a bit like paintbrush marks. This is known as rain scald and is treated in a similar way to uncomplicated mud fever.
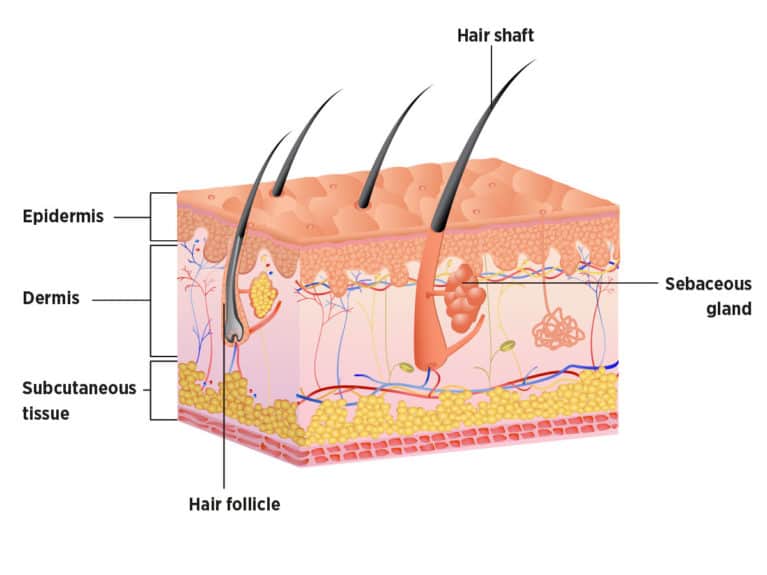
Skin structure
The skin is made up of an outer epidermis, a middle dermis and an inner subcutaneous layer. The outer epidermal layer acts as a physical barrier to the environment. If it is damaged, this allows bacteria to infiltrate the skin, starting an infection and inflammatory reaction. The skin is also protected by hair follicles that grow from the dermis, and these have sebaceous glands that produce natural oils to help waterproof and protect the skin.
It is normal for the skin of a healthy horse to have many micro-organisms (bacteria and fungus) living on its surface, causing no harm. It’s when they get under the skin, enter the deeper layers and multiply that problems occur.
Clear as mud
If the skin is damaged in any way, micro-organisms can take a hold and cause infection. Apart from Dermatophilus congolensis, which is found in soil, other bacteria can also be found in mud fever lesions, such as Staphylococcus and Pseudomonas, as well as mites and fungi. Other causes of mud fever include…
- Leg mites (Chorioptic mange) can create damage and cause thickening of the skin, predisposing it to bacterial entry. They irritate the skin and lead to scratching, allowing bacterial infection to establish. Horses with leg mites are often very itchy and stamp their feet, and they may even bite and scratch their limbs. The mud fever will not improve if the mites aren’t treated, too. Mites are common in breeds with feathered legs, and a diagnosis of mite infestation can usually be suspected from the breed type and clinical signs. A definitive diagnosis is made by taking deep dermal skin scrapes from the edges of lesions.
- Wet conditions cause the skin to soften. Mud will rub against this softened skin causing abrasions to the surface, and certain soils and pastures appear to be more likely to cause skin damage than others.
- Lots of work in sandy arenas can be traumatic to the skin.
- Pasture with copious rough vegetation or spiky weeds can cause skin damage.
- Excessive leg washing weakens the skin and removes the natural grease that acts as a barrier, resulting in cracks that can allow the entry of bacteria.
- Certain bedding can act as an irritant, both physically (straw) or chemically (high ammonia from urine in deep litter).
- Boots and bandages incorrectly placed or inappropriately used can cause damage to the skin barrier.
- Pastern and cannon leukocytoclastic vasculitis are immune-mediated conditions that can look very similar to mud fever and can predispose a horse to bacterial infection. They are usually seen in the summer and are thought to be allergic reactions to either sunlight or something in the environment, such as buttercups, other flowers or plants, or bedding. They cause reddening of the skin around the pastern above the heel bulbs, and tend to be seen on white legs. They cause oozing of serum and scabs that are often very painful to touch.
- Sunburn or photosensitisation on areas of pink skin on the legs. Photosensitisation can be caused by ingestion of certain plants, such as St John’s Wort, and liver problems. It causes the skin to become ultra-sensitive to sunlight, leading to raw, oozing areas of skin that become crusty and then slough away. The damage caused to the skin enables bacteria to enter.
- Pemphigus foliaceous is a very rare auto-immune condition that also causes crusting and scabby legs, with or without itching, often around junctions of skin and horn – for example, the coronet band and chestnuts. This condition causes the body to attack itself, again leaving the skin vulnerable to infection. It can be diagnosed with a biopsy.
Diseases such as PPID (Cushing’s disease) can reduce your horse’s immune system, making it easier for bacteria to gain a hold.
Fever relievers
Most mild cases of mud fever can be treated without having to contact your vet first, unless you need advice or you think there may be an underlying cause that needs treatment. The basis is to treat any underlying conditions, such as mite infection or contact allergy, remove the infection and then allow the skin’s natural barrier to heal.
Usually, this will involve stabling your horse to protect him from mud contamination and the wet-dry cycle that damages the skin barrier. Turnout in an arena may be possible if it is dry, but sand can be an irritant and your horse may still get chapped skin.
Heavily feathered horses will benefit from having their legs clipped. This allows easy visualisation of the area affected, and permits the hair and skin to dry faster. In addition, the scabs will come away more easily from the affected part and topical treatments can reach the necessary areas, rather than being stuck in the hair.
Traditionally, bacteria were thought to live within the scabs and, therefore, by removing them we would remove bacteria from the site. However, we now understand that D. congolensis is an anaerobic bacteria (it cannot survive in the presence of oxygen) that is usually found living underneath the scabs. Consequently, scab removal is still important as it allows oxygen to the affected area as well as facilitating effective cleaning with anti-bacterial solutions. Here’s how to do it…
- Soak your horse’s legs in warm water and dilute Hibiscrub (chlorhexidine), then remove any scabs that come away easily without forcing them. Hibiscrub has excellent antibacterial and some antifungal properties, if used appropriately. It should never be used neat – the ideal dilution is 0.1% and your vet can advise you how to dilute it appropriately, as it can be bought in different strengths.
- Rinse his legs well with warm water.
- Use clean towels to dry his legs thoroughly afterwards. Ideally use a different towel for each leg, to avoid spreading the infection around.
- Antibacterial cream such as silver sulfadiazine (flamazine) may be applied daily and after washing his legs.
Repeat the scab removal process every 3–4 days. Doing so more often will dry out the skin too much.
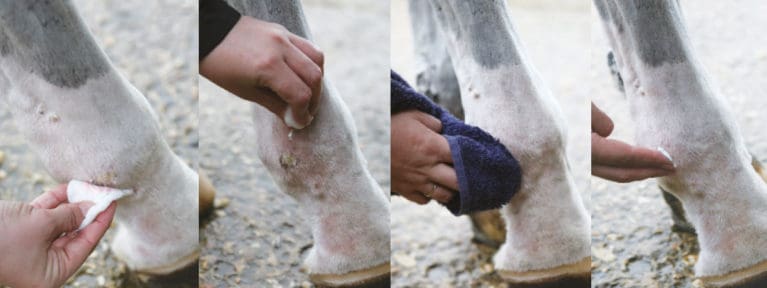
A closer look
If after a couple of weeks the mud fever isn’t improving or has worsened, it’s time to call your vet. They will want to examine your horse, and will ask you lots of questions regarding his management and whether there are other horses on the yard who are affected or have mites.
Your vet may want to take acetate tape impressions – where tape is pressed against the skin, sticky side down, and the particles attached to it are examined under a microscope – or hair samples to look for fungal or bacterial infection. They may also collect some of the scabs for examination or culture for bacteria, or want to take a skin scrape using a scalpel blade to look for mites, which burrow through the skin.
Veterinary treatment for mud fever varies depending on the cause. There are many treatments available and no one is a cure-all. Some treatments that your vet may prescribe on a case by case basis include…
- Systemic antibiotics – given orally or by injection, courses can vary from three days to three weeks and will be determined by your vet
- Topical antibiotics can be applied to the affected site as a cream
- Pain relief and anti-inflammatories are important if your horse has painful scabs. Making him more comfortable is important for his welfare, but is also likely to make him more compliant when it comes to removing the scabs or applying treatment
- Mite treatments for mite infestations
- Stabling during the day or using ultraviolet turnout socks for horses with light-sensitive lesions
- Steroids for horses who have immune-mediated conditions
If the condition does not respond to treatment, or your the vet is suspicious of a neoplastic lesion (tumour or sarcoid) or an immune mediated condition (pastern and cannon leukocytoclastic vasculitis or pemphigus foliaceous), they may decide to take a full thickness skin biopsy. This will be sent to a laboratory, where the structure of the skin cells and layers will be examined under a microscope by a specialist.
Prevention and prognosis
Although mud fever is traditionally associated with mud coating the legs, many horses who live in muddy fields continue through the whole winter without developing any signs of the condition. This leads us to believe that it is not just the mud, but instead the constant wetting and chilling of the skin that is at the root of the problem.
This theory is supported by the fact that mud fever can often be a real issue on yards where the horses’ legs are washed on a frequent basis throughout the winter months and left wet for long periods of time, whereas yards that never wash horses’ legs rarely suffer with mud fever.
In most cases, the prognosis for a full recovery is very good, providing that the appropriate treatment is carried out. However, mud fever can be tricky to treat and take a while to clear up, so the best course of action is to prevent it occurring in the first place. The following tips will help you keep the problem at bay…
- Rather than daily washing, a better course of action is to leave the mud to dry naturally on the legs, then brush it off
- Leaving the lower legs unclipped was thought to protect them from infection, but we now realise that mud fever is more common in horses with hairier legs, because they take longer to dry out and it is very difficult to identify early lesions, so trimming them up is a good idea
- Waterproofing the lower limbs, particularly before turnout or exercise, is good practice. Barrier creams such as Sudocrem, are effective for this. However, it is important to ensure that your horse’s legs are clean and dry before application, otherwise the area between the wet skin and the greasy cream will provide the perfect breeding ground for bacteria
- The rotation of paddocks to avoid poaching and the use of electric fencing to block off particularly muddy areas, such as those around gateways, will help to minimise the risk of mud fever